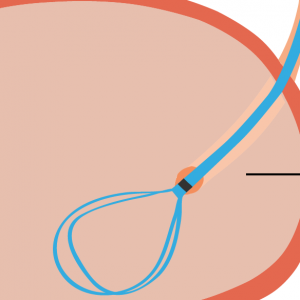
 For most patients who have ever experienced a ureteral stent, the faster the stent is removed and becomes a part of their past history, the better. A look at our ongoing stent (dis)comfort poll makes this clear. With a total of 1,716 people responding, 59% reported that the pain level from their stent was 8 or higher on a scale of 1 to 10.
For most patients who have ever experienced a ureteral stent, the faster the stent is removed and becomes a part of their past history, the better. A look at our ongoing stent (dis)comfort poll makes this clear. With a total of 1,716 people responding, 59% reported that the pain level from their stent was 8 or higher on a scale of 1 to 10.
In honor of putting stents in the past tense, we decided to look back at the long history of ureteral stents, starting way back in the 1800s with the first reported placement of a tube into a ureter and finishing up with the introduction of an all metal (!) stent in 2006. Read on to find out more.
1800s– Dr. Gustav Simon describes inserting a tube into a ureter during open bladder surgery. He is credited with being the first person to “stent” a ureter.
1900s– Dr. Joaquin Albarrano creates first catheter meant to be used in the ureter. Stents at that time were typically made of fabric covered in lacquer varnish.
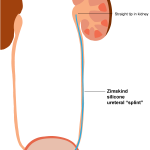 1967– Dr. Paul Zimskind reports insertion a straight silicone tube into a ureter to relieve obstruction. In their report, they referred to the device as a “ureteral splint”. This is the first use of a stent that is placed endoscopically (using a camera) instead of through an open incision. It represents the beginning of the modern era of ureteral stents. However, because the stent is straight, it is prone to accidentally slipping out.
1967– Dr. Paul Zimskind reports insertion a straight silicone tube into a ureter to relieve obstruction. In their report, they referred to the device as a “ureteral splint”. This is the first use of a stent that is placed endoscopically (using a camera) instead of through an open incision. It represents the beginning of the modern era of ureteral stents. However, because the stent is straight, it is prone to accidentally slipping out.
1973– Dr. James Montie coins the term “stent” to refer to indwelling tubes placed in the urinary tract.
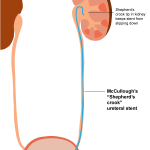 1974– McCullough describes the use of a “shepherds crook” stent to prevent the stent from slipping down and out of the kidney. The shepherds crook design was borrowed from existing stents meant for insertion into blood vessels. While the stent no longer migrated downwards thanks to the upper curl, it was still prone to slipping upwards into the kidney.
1974– McCullough describes the use of a “shepherds crook” stent to prevent the stent from slipping down and out of the kidney. The shepherds crook design was borrowed from existing stents meant for insertion into blood vessels. While the stent no longer migrated downwards thanks to the upper curl, it was still prone to slipping upwards into the kidney.
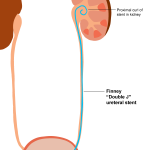 1978– Finney introduces the new “Double-J” ureteral stent design, which has a curl at both the top and bottom of the stent. This is now the most common type of stent used. Having a curl at both ends of the stent helps to prevent the stent from slipping either upwards or downwards. Modern stent designs having a full curl instead of just a “j” curl are technically called “pigtails” but the term double-j is still used interchangeably.
1978– Finney introduces the new “Double-J” ureteral stent design, which has a curl at both the top and bottom of the stent. This is now the most common type of stent used. Having a curl at both ends of the stent helps to prevent the stent from slipping either upwards or downwards. Modern stent designs having a full curl instead of just a “j” curl are technically called “pigtails” but the term double-j is still used interchangeably.
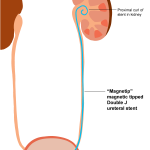 1989– A magnetic tipped “Magnetip” double J ureteral stent is introduced by ACMI which can be removed using a magnet instead of by cystoscopy (insertion of a camera). However, it is no longer on the market, probably because removal using a “Magnetriever” was not always reliable. In one study, only 86% of stents were removed successfully. The others required traditional cystoscopy for removal.
1989– A magnetic tipped “Magnetip” double J ureteral stent is introduced by ACMI which can be removed using a magnet instead of by cystoscopy (insertion of a camera). However, it is no longer on the market, probably because removal using a “Magnetriever” was not always reliable. In one study, only 86% of stents were removed successfully. The others required traditional cystoscopy for removal.
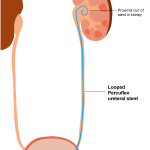 2000– Based on the concept that the distal curl of the stent in the bladder is the cause of patient discomfort, a stent with loops of loose plastic strings at the distal end is introduced by Boston Scientific. The Percuflex “tail” stent was designed to have less plastic material in the bladder. In research studies, it was not found to always be better in terms of discomfort. Dunn and colleagues reported fewer bladder symptoms in patients with the tail stent placed in a study published in 2000 but Lingeman and colleagues in 2009 found no differences in discomfort at postoperative day 4.
2000– Based on the concept that the distal curl of the stent in the bladder is the cause of patient discomfort, a stent with loops of loose plastic strings at the distal end is introduced by Boston Scientific. The Percuflex “tail” stent was designed to have less plastic material in the bladder. In research studies, it was not found to always be better in terms of discomfort. Dunn and colleagues reported fewer bladder symptoms in patients with the tail stent placed in a study published in 2000 but Lingeman and colleagues in 2009 found no differences in discomfort at postoperative day 4.
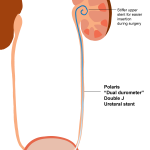 2001– A ureteral stent made with softer plastic on the lower end and stiffer plastic on the upper end is introduced to improve comfort by Boston Scientific. The advantage of having a stiffer upper end is to make insertion during surgery easier, which can be difficult if the stent is too soft along its entire length. The softer bottom end is in contact with the bladder and theoretically might make the stent more comfortable for patients. However, the Polaris dual durometer stent was not able to reduce patient discomfort in a study by Davenport and colleagues published in 2011.
2001– A ureteral stent made with softer plastic on the lower end and stiffer plastic on the upper end is introduced to improve comfort by Boston Scientific. The advantage of having a stiffer upper end is to make insertion during surgery easier, which can be difficult if the stent is too soft along its entire length. The softer bottom end is in contact with the bladder and theoretically might make the stent more comfortable for patients. However, the Polaris dual durometer stent was not able to reduce patient discomfort in a study by Davenport and colleagues published in 2011.
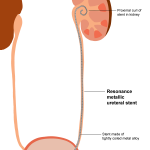 2006– The Resonance metallic stent is introduced by Cook. It is made of a continuous coil of metal, similar in appearance to a tight spring. It has curls at both ends and is designed to be stronger in order to resist kinking or collapse from inwards pressure coming from outside the ureter. The most common use of this type of stent is for ureteral blockage from cancers such as cervical or colon cancer which can sometimes compress the ureter from direct growth surrounding the ureter.
2006– The Resonance metallic stent is introduced by Cook. It is made of a continuous coil of metal, similar in appearance to a tight spring. It has curls at both ends and is designed to be stronger in order to resist kinking or collapse from inwards pressure coming from outside the ureter. The most common use of this type of stent is for ureteral blockage from cancers such as cervical or colon cancer which can sometimes compress the ureter from direct growth surrounding the ureter.
The future– Researchers are experimenting with new stent designs in an effort to make them more comfortable and to avoid the necessity of removing them. These new stents include designs that are impregnated with medications directly in the stent that can relieve discomfort and biodegradable stents that are absorbed over time. We’ll cover these and other new stent designs in a future post.
References:
Clinical effectiveness of a new stent design: randomized single-blind comparison of tail and double pigtail stents. Journal of Endourology, 2000, Dunn et al.
Assessing the impact of ureteral stent design on patient comfort. Journal of Urology, 2009, Lingeman et al.
New ureteral stent design does not improve patient quality of life: a randomized, controlled trial. Journal of Urology, 2011, Davenport et al.
Update on ureteral stents, Urology, 2004, Lam and Gupta
Ureteral stents, AUA update series 2008, Vignall and Denstedt
I had 4 mm kidney stone removed on Thursday via a basket. Though I told the urologist that I didn’t want a stent, and though the surgery was uncomplicated, I got a stent anyway. It won’t be removed until next week! It’s very painful, causing spasms in my ureter and kidney. I’ve been bleeding heavy for four days. I feel that it has complicated my recovery and lessened my quality of life. I’ve had stones removed before through the basket retrieval method, and though I usually have a bad day, I recover much more quickly.
I had laser lithotripsy and stent placement on my right side last week, got my stent removed this morning in the urologist’s office. Honestly, if I ever have to do this again, I would run, not walk, to the hospital to have it done. BEST THING EVER to happen to me. The surgery, done under general anesthesia, was ridiculously easy, had bladder pain, urinary urgency and mild incontience the whole 10 days my stent was in, but that’s nothing compared to the weeks of debilitating stone attacks. That was easy to deal with, the urologist numbed my urethra before removing the stent and that took all of 30 seconds if that, and it was fun to watch him do it on the screen. No pain, extremely easy, no after effects, and no more bladder pain, urinary urgency and mild incontinence, either, but those were more inconvenient than anything else. I’ll take those over stone attacks every day of the week.
An excellent surgeon like what I had makes a WORLD of difference! I highly recommend laser lithotripsy and stent placement surgery. Trust me, you will bless the day they insert your stent, best thing ever. Beats chronic stone attacks every day! I loved having it in, also glad to have it out. On to a healthier life and a better diet. Thank you to my surgeon and my local hospital. They totally rock!
It seems most of the comments are about all the problems patients have experienced. This frightened me enough that I delayed having the stone removed until it was clear it wasn’t going to pass on its own. While I can’t say the experience with the laser lithotripsy and the subsequent stent was no big deal, it was tolerable. (With heavy duty pain meds!) I think every patient, every stone and every doctor is different. If you are fortunate like I was, you will survive. If you are less fortunate, it will be a real trauma. The only advice I can give once you are diagnosed with a stone is to take the pain meds and take them before the pain is overwhelming. Also, if possible, have someone with you to help make decisions and argue with the doctors if necessary. This is very hard to do when your brain is clouded with pain and/or pain medication.
I don’t have stones but I have a tumour pressing on my ureter. I was unfortunate enough to have stents inserted through my back under local anaesthetic. The pain was incredible and I sobbed uncontrollably after the second one was put in. The stents have been ok for three weeks but now I have pain in my left kidney when I empty my bladder. I will have these stents in for up to six months whilst I have chemo. If the tumour doesn’t shrink, I will have to have stents removed and replaced for the rest of my life. What a lovely thought, eh?
Hello Everyone, All I can say is, if you ever need to have stents placed in your ureter for stones, go to Licking Memorial Hospital in Newark, Ohio. I went to the hospital on an emergency basis, septic and with both kidneys completely shut down. They operated on me within a few hours after arriving and placed two stents in my kidneys due to lots of blockage from large stones (14 mm). I was in the hospital for 5 days and when I left, I never had one pain from the stents. They’ve been in now for nearly 6 weeks (coming out in the next couple of weeks) and I’ve had no pain or discomfort at all from the stents. Out of three or four large stones, I’ve passed all but one large (14 mm) stone and they are making plans to remove it along with the stents. The only question I have is: when I went into the ER (and this includes the 15+ years prior to this incident) I had huge, swollen, feet, ankles and legs. I’m 150 lbs. overweight, have been checked for PAD and other heart related problems, but have been given a clean bill of health along those lines. No one knew what was causing the swelling. My family doctor kept telling me it was because I’m overweight. But when I went into the ER for my kidney stones, literally 36 hours after having the stents placed, my feet, legs and ankles, deflated to an almost “skinny” size. I literally had wrinkly skin on my feet, and they’ve stayed that way since. So my question is……when they take out my stents, will my feet, ankles and legs swell back up again? I have to believe (given the 36 hours it took for them to go down) that putting the stents in my kidneys are what removed this 15+ year swollen effect. But will it return when they are removed?
I’ve had two stones that had to be removed by laser lithotripsy. The first was about five years ago. After the surgery, the doctor informed me that he couldn’t remove the stone because of inflammation in the ureter and placed a stent in the ureter. An hour or two after I got home I was in the worst pain of my life. I wasn’t told that this could happen. I called the doctor and he basically said that this was normal. I also had extreme burning when I urinated and blood leaking out after. My penis looked and felt like a dog had been chewing on it. The pain gradually eased after about a day and a half and the stent was annoying but not really painfull for the next three weeks. The stent was then removed and the stone was broken up. I asked the doctor not to reinsert the stent unless it was absolutely necessary and much to my surprise when I woke up he told me that he did not.
I had the second lithotripsy a week ago, about two months after the stone had me in the ER. Different doctor. Better experience. I couldn’t talk him out of the stent but I told him about my first stent experience he said that the pain was probably bladder spasms and that Percoset could make it worse. He gave me Oxybutynin for the spasms and I didn’t have as much pain from the stent. I did have the extreme burning when urinating followed by four of five drops of blood after I stopped. This cleared up after about twelve or sixteen hours. After that the stent was annoying but not painful.
The stent was removed today in the office. I was terrified but the anticipation was much worse than the proceedure. Not much worse than having an IV put in. The nurse put numbing gell in and after about ten minutes the doctor started. It only took about thirty seconds. It hurt when the scope pushed into the bladder and when the stent started out but not that bad and only for a second. Very little discomfort afterwards. If I have to have it done again l’ll have it done the same way by the same doctor.
Kidney stones are like snowflakes. No two are alike.
Hello. I had my first lithotripsy and stent planet on July 1,2015. Is scheduled for a follow-up on the 16 th. 2 days before I went on for my X-ray, which there doctor office never sent the order to the lab for. Those fee days before the follow-up I was in so much pain that I risked my job by taking my pain meds while operating heavy equipment. When I went to follow-up I begged him to take the stent out! He asked me the X-ray which explained all the pain I was in. The stent’s guidewires feel it off my kidney and literally were sitting at the opening. The good news was the stone was all broken up but about 50+ fragments were stuck in the uterar. He scheduled me for an emergency surgery the next day to replace the stent and use a laser to remove the rest of the stone. He said follow-up in a week. That surgery was 7-17-15. First available appointment is August 11! So I have to have this in for an additional 3 weeks hoping that I don’t have a repeat of before. I will never get another stent again!
I have suffered with stones many times over the years and have endured several cystoscopes. I have had laser surgery to blast one to many pieces so I would be able to pass it. And with my last kidney stone surgery the Dr placed stents in both of my ureters. I was unaware that this procedure was being done until I woke up in recovery in severe pain. The Dr informed me he had removed the stone and the stents were placed to help with the passing of any other stones that I may have had. So I went home with my pain meds and my antibiotics expecting the pain to ease up by the next day thinking it was caused from the surgery. But by the next day the pain was worse so I called the
Dr office and reported the pain I was experiencing. I was told per the nurse that this was normal. That my body was trying to adjust to a foreign body being there. So I continued with my pain medicine and was having no relief at all and by the next day the pain was almost unbearable. So I call the Dr office back. I was told the same thing by the nurse and that it would get better when my body for accustomed to the stents. By the fourth day I was in So much pain I was unable to get out of bed. I called the Dr office again. This time I was told that my body was rejecting them and that my body was trying to push the stents out. I begged to come into the office and have them removed with No luckn. I was told they had to stay in for two weeks and that if I needed more pain medicine I could come into the office and pick up a new rx. Which I was unable to do bc the pain was so bad. My son had to go for me and have it filled. I almost overdosed from the pain medication bc I was in so much pain that I would take one of the pills and then maybe doze off for a little while. And when I awakened I would take another pain pill. It got to the point that I knew I had taken too much pain medication when I realized that the times I was able to doze off had only been for a few mminutes at a time. And I was thinking I had been asleep several hours. That’s how bad I hurt and how tired I was. So I actually had to put a tablet in my bed and every time I took a pain pill I would write down the time so that when I woke up I had to make sure at least four hours had passed. For ten days I was unable to get out of bed bc of the severe pain I was having it felt like I was in labor the whole ten days. They took them out four days early in the Dr office with no sedation and nothing at all for pain. And after three attempts at removing the stents with no luck the Dr realized the machine he was using to remove the stents was broken. He then have me something for pain and sent me over to the hospital to have them removed. I am now facing another surgery for a 6mm stone in my left ureter and wanted me to sign paperwork for stent insertion past surgery which I refused to do. So now I am just waiting for this stone to pass and it has been about three months. I am passing so much blood in my urine that I’m concerned my blood count is low. Every time I pee there is so much blood that my urine looks almost black my suggestion is if you have a choice DO NOT GET STENTS
My experience with a stent was completely opposite and I have one in right now. while being annoying it didn’t last.
I’m sorry your experience was so bad.
Hello all.
So I have been dealing with non obstructive upper lobe of right kidney. Had first procedure on April 17 and had two stents inserted to stretch the tubes so the damn in trumpets would be able to get to the stone.
Problem one: The pain for three days was down right awful. Everytime I would urinate my kidney felt like it was cramping and send me to my knees. Lots of pain meds.
Problem two: Continued to urinate blood way beyond the two to three days I was told.
Called DR and was given two meds for urgency and spasms.
Problem three: Started feeling really sick by end of week one. Saw the nurse practitioner and was put on antibiotics.
Went for pre administration for second procedure and had urine culture.
Problem four: urine showed multiple issues and my urologists ignored them and performed the stone removal procedure and related the Stent and I have been getting sicker by the day.
Called the DR who finally called me back and wanted to throat punch him at this point. He decided maybe I need another antibiotic. Let me explain. I called the office because I spiked a fever overnight that went above the 101 that they use as a threshold. Was told take ibuprofen and since I was having the Stent removed the next day he would do another urine culture. Even though I felt like a semi played demolition derby with me I had my roommate took me to the surgery center where upon taking my temp it was 100.5. Not overly high but persistent. Had chills and was wrapped in warm blankets.
When I finally saw DR gonna get a throat punch he said and I quote you look like you don’t feel well. Did yet another urine culture after cancelling the procedure. Then was asked by this clown if I needed to go to the ER. Really you are a GD DR and you are asking me. How about maybe making a medical decision being that’s what you are being paid to do.
So I lay here in bed fighting fevers, chills and sweats. Feeling like a train wreck while I wait for DR to call me with results. Not. Going to ER before my kidney decides to fail.
Had 2 stones removed last fall. I am due for my 6 month check and am all of a sudden having some symptoms again. No way will I allow a stent again. It only stayed in for about 72 hours and then partially “fell out”, folded in half. I removed it myself which hurt like he** and then OMG the pain from a kidney spasm. I was nearly on the floor and I have high pain tolerance. Also urinating through a urethra irritated by a plastic wire folded in half was worse than giving birth. I have followed the dietary suggestions quite well so am not really happy to have more symptoms…we’ll see what next week brings but it will not bring a stent.
I had a stone but stuck in the tube between kidney and bladder .the doctor had open surgery to get out stone and placed a artificial tube in the uriter after 10 days the tube had to remove and doctor used a stent for that purpose. Now I,m feeling pain sometimes in urethra which might be crashed by stent. After four year for surgery.
Going in for the second time in the last four years, this time I am having a Ureteroscopyy on my left side.. and he said he would be using a stent again. Last time I had my stent out about a hour after I was home the pain was so bad I almost called 911. The doctor did not tell me this could happen. So of course not in any way looking forward to the days ahead. Has anyone had a Ureteroscopyy and how long did it take you to feel better? Any help is great I almost don’t even want to go through with it.
hi fellow stentors I recently have undergone a pcnl for a complex kidney stone I have had a stint in the past when they did lipotripsy to try to remove it I had the stent for 3 months and it was a long 3 months I experience at lot of pressure and pain at times I would wake up at night in a sweat and feeling it was very uncomfortable I read some posts that it helps to drink water and it doesa heating pad and ice sometimes helps too I never wanted another but I was told with the PCNL surgery is that I would have one for a week well with surgery they had to do more than just normal and now I have two of them for 3 weeks side by side and really I thought one was unpleasant two of them is doubled the pressure and the pain I didn’t even know 2 side by side was possable
I passed by first stone in 1988 and have been passing them ever since.
I have reduced the size of the stones by hydration, dietary restrictions and exercise. Several years ago I can across an article that I can no longer locate. I believe it was in the New England Journal of Medicine that opined that a stent was normally unnecessary after a kidney stone procedure. However, the practice has continued to insert one. Is anyone familiar with the argument that a stent is not really necessary?
Monday, August 18th PM, I went to the ER with severe pain, I now know it was a 9.4mm kidney stone. I was finally admitted to a room by 2:30am; I had surgery for a stent Tuesday night and I was released the next afternoon.
This past Tuesday I had lithotripsy. Once I had the stent removed, the following day, I started passing stones. Until then, I was passing granules of sand.
That being said, I was told that the stent was necessary because of the size of the stone, and how high it was. They could not do lithotripsy right away because my white blood cell count had gone up, and they couldn’t risk it. I guess it is more case by case basis. Up there with the pain I have from the stones themselves, having that stent removed was AWFUL.
I know this is an old post, but yes, I’ve read studies that concluded that most stents are not necessary. The urology office I’m seeing routinely gives patients stents with a ureteroscopy to remove a stone. It makes me wonder if doctors are giving patients stents to make more money. They not only bill insurance for the stent placement but also for it’s removal.
This is in no way a criticism of all urologists! I’m am absolutely sure there are many qualified, caring professionals available to treat kidney stones.
At 45, I recently experienced my first kidney stone, and hopefully my last! My experience began with no problems, no pain, just some blood in my urine for the first few days. But on the third day the pain hit and I was truly not prepared. Some of this was because I had never experienced it, but some of it unfortunately was because my doctor(s) did not discuss it with me at all. After a trip to the ER, and some much needed pain medication, I had the 6mm stone removed and a stent placed. I was told I would probably only have slight discomfort when urinating, if anything at all, and that I could remove the stent myself in 2-3 days. I began to noticed some edema, but thought it was probably normal considering the anesthesia from the procedure. Two days after the procedure, I returned to work, and within hours I was noticeably more bloated, and getting bigger by the hour. I began to feel really bad. Some pain, not horrible, mostly just very unwell. I contacted my doctor, who referred me to the urologist, who referred me to urgent care. When I got to urgent care, the doctor took a look at me and compared my weight to what it had been only 5 days earlier, and sent me directly to the hospital. After a few hours and a ct scan I was told that I had ascites and that it was most likely either a ruptured ureter or that one of my kidneys was failing…..within an hour, and after a phone consult with the urologist that changed to …Your constipated! I was cathed, literally stuffed with laxatives, sent home & told to go to the urologist first thing in the am…by the time I got to the doctor the next morning I was so sick. But once again, I was sent home with directions for laxatives….I became so ill later that night, I truly thought I was dying. I was terrified, and the pain was worse than with the stone itself. I went back to the ER. Finally I was admitted, but once again given laxatives….at this point I had drank 3 bottles of Mag citrate, endured several suppositories, and was being given stool softeners like candy. Also, during this time, my BP continued to rise, at one point to close to 150 over 90. I was too sick to put up a fight, but there was no result from the laxatives, and I was coherent enough to refuse an enema. I was experiencing severe flank pain, radiating around to my groin and down my leg. The entire time I was concerned about the stent. I thought something had to have gone wrong. The Urologist refused to do anything until after the weekend, so I spent 4 days in the hospital. Finally Monday morning the stent was removed, and I was sent home. The edema has improved significantly! I’ve lost over 10 lbs., and despite all the laxatives I was given, there was no huge result. They obviously had some effect, but I was clearly not that constipated, if at all. In all I gained over 14 pounds in 5 days. I was 123lbs the day my symptoms began….by the time I entered the hospital, I was 139.6! I was discharged with the diagnosis of constipation, which truthfully infuriates me. I wasn’t even eating. Even the nurses at the hospital were outwardly in disbelief of what was being said of my condition. After all was said and done, I believe my body had a Hyper-Immune response to the stent. I think it was simply rejecting it as a foreign body, and the swelling was a symptom of that. I can’t seem to figure out why the urologist refused to consider it as a possibility. Every time I raised the possibility, I was shut down completely. I have committed myself to doing everything possible to avoid another kidney stone, but I realize there aren’t any guarantees. If I ever experience another, I will make sure the doctors know of this experience, and do all I can to avoid another stent placement.
I had a stone removed on September 2,2014. I had a stent and had horrible pain for two days after my procedure. They removed it! It now is two months later and I still have discomfort where the stent was and in my kidney. It is not all the time ,but enough that I am concerned something is messed up! I was told the stone was destroyed as planned,but remnants remained.