Many people have ureteral stents placed to prevent or treat urinary tract obstruction, and if you happen to be one of these people, it’s likely that you’re familiar with some of the symptoms of having a stent. However, it can be easy to forget that you have a stent in place, particularly if you’re experiencing minimal discomfort from your stent. Generally, it is recommended that stents be removed or exchanged before every 3-4 months. But what happens if you have it in place longer than this or if your stent is forgotten?
One of the most common things that may happen to ureteral stents is encrustation, in which calcifications form around the placed stent. This phenomenon occurs to a minor degree in many patients and is usually of little consequence. It is most extensive when the stent is left in place for too long, and urinary tract obstruction and infection may occur as a result of encrustation. The amount of stent encrustation is directly related to how long a ureteral stent has remained in place. One study found that 9.2% of stents became encrusted when in place for less than 6 weeks, while 47.5% of stents that remained in place for 6 to 12 weeks were encrusted and 76.3% of stents were encrusted after 12 weeks (El-Faqih et al, 1991). The length of time a stent remains in place is in fact the greatest risk factor for stent encrustation. Other risk factors include the composition of the stent used, a history of stone formation, urinary infections, alkaline urine, and pregnancy. Because of the physiologic changes accompanying pregnancy that predispose these patients to more profound indwelling ureteral stent encrustation, it is recommended that stents are removed or exchanged every 6-8 weeks in pregnant women (Kavoussi et al, 1992).
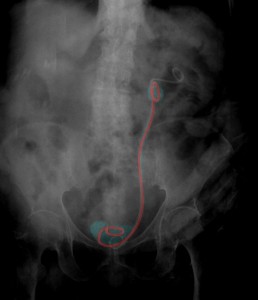
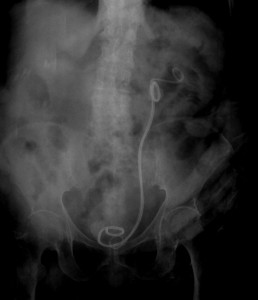
Xray illustration of retained left ureteral stent. Stent highlighted red. Surrounding stone highlighted blue.
Proximal stent migration and fragmentation are two other complications of indwelling ureteral stents. The hardening and degradation of stent polymers may lead to fragmentation, particularly if the stent is left in place for longer than 6 months (Monga et al, 1995). Uncommonly, a stent may perforate the ureter or erode through the ureter and form an abnormal connection between the ureter and adjacent structures. The occurrence of these complications is associated with an increased amount of time that the stent is in place.
If a retained ureteral stent is suspected, your doctor will likely obtain imaging of your urinary tract to determine stent location, the extent of encrustation and to help quantify stone burden, a prognostic indicator that helps to determine correct surgical management. Because the composition of the encrustation is typically calcium-based, most can be seen on a plain film x-ray of the kidneys, ureters, and bladder. CT scans or ultrasonography are other useful imaging modalities, particularly if the stones are composed of uric acid and cannot be seen on an x-ray. Radionucleotide studies may be necessary if the stone burden is high to assess kidney function. Depending on the extent of encrustation, the stent may be removed in a retrograde fashion by cystoscopy with or without extracorporeal shock wave lithotripsy (ESWL). If more extensive encrustation is present, transurethral cystolitholapaxy, retrograde ureteroscopy and laser lithotripsy, or antegrade nephroscopy and ureteroscopy may be preformed. In some cases, multiple sessions are required to completely remove the stent and stones. Antibiotics may be given if an infection is present.
Recognizing the temporary nature of an indwelling ureteral stent and the need for timely follow-up with your urologist is the best way to prevent the complications associated with stent retention. The management of retained ureteral stents is associated with a 6.9-fold increase in financial burden compared to the average cost of timely stent extraction (Sancaktutar et al, 2011). Recently, the development of electronic stent registries at some hospitals to monitor stent placement and removal has shown to significantly reduce the number of forgotten stents (Lynch et al, 2007).
References
El-Faqih, S. R., Shamsuddin, A. B., Chakrabarti, A., Atassi, R., Kardar, A. H., Osman, M. K., and Husain, I. Polyurethane internal stents in treatment of stone patients: morbidity related to indwelling times. J. Urol., 146: 1487, 1991.
Kavoussi, L. R., Albala, D. M., Basler, J. W., Apte, S., and Clayman, R. V. Percutaneous management of urolithiasis during pregnancy. J. Urol. 148: 1069-1071, 1992.
Lynch, M. F., Ghani, K. R., Frost, I., and Anson, K. M. Preventing the forgotten ureteral stent: implementation of a web-based stent registry with automatic recall application. Urol. 70: 426-426, 2007.
Monga, M., Klein, E., Castaneda-Zuniga, W. R., and Thomas, R. The forgotten indwelling ureteral stent: a urological dilemma. J. Urol. 153: 1817-1819, 1995.
Sancaktutar, A. A., Soylemez, H., Bozkurt, Y., Penbegul, N., and Atar, M. Treatment of forgotten ureteral stents: how much does it really cost? A cost-effectiveness study in 27 patients. Urol. Res.; DOI: 10.1007/s00240-011-0409-3, 2011.
Vanderbrink, B. A., Rastinehad, A. R., Ost, M. C., Smith, A. D. Encrusted urinary stents: evaluation and endourologic management. J. Endourol., 22(5): 905-912, 2008.
will it hurt me if i dont get my stents taking out
I had a stint placed in 2008 and wasn’t aware that when they removed it it would cost me 600.00 which I didn’t have and couldn’t afford better insurance to cover the cost. So I had no choice but to leave it in. A year passed and I could walk it felt as if a stick was driving out of my urethra Fromm the inside out I would have to stop n have my family grabbed the car so I didn’t have to walk across the parking lot. Eventually it caused a blockage from my kidney to my bladder causing s3ver bladder infections and my urine smelt so potent of this up it made people freak out when they went into the bathroom after me.. That went on for a few months then there’d side pain began again but 20 times worse then your kidney stone pain… I went to the hospital and they explained that my kidney had been sitting in my swampy urine and all the bacteria with it causing my kidney to swell massively they had to put me under zip off the calcium around the stint so they could remove it and then put another one in to drain the calcium from my bladder. Then 2 weeks went by and I had them pull the 2nd one from the office… Never had a problem until the other day 05/18 went to hospital thought I had a stone and the Dr told me my kidney has shrunk slot from 2009 but still is swollen causing slot of urinary tract infections. I’m scared to find out all I know is I am drinking g tons of water now…. It’s scary things cannhappen just listen to the doctors n the stuff they say is important don’t leave it in it will cause serious problems for along time if not taken seriously
Tiffany
this is exactly what im feeling now, ive had a stent in place for almost a year now and i feel like theres a needle in my urethra. i cant walk, sit or even stand without being in pain. i also couldnt afford to have it taken out and have my kidney stone taken out. so i kept it in. i want to go to the hospital but im scared they wont help me because i dont have money to pay. i really cant take the pain anymore.
I could never forget, the pain always reminds me each and every day. The doctorss/hospital/urology on the other hand – they forgot. They said one month and they would remove it – liars. It’s been four months now and it’s ruining my life. 7 more days until I get it removed…
It’s Saturday and I had laser lithotripsy and stent placement surgery on Tuesday. Today is the first day since surgery that I don’t even know that my stent is even in there. All pain and discomfort are totally gone. I’m extremely happy to have a stent, it feels really very good in there, and I’m scared to death to get it out (they want me to keep it in for at least two weeks post-op). Since its dilating my ureter, it feels like security against anymore stone attacks, but I know that it’s eventually gotta go.
How long can I safely keep it in with no complications? I’m eager to keep it for a while, because after five stone attacks in two weeks time, I’m sure that I’ve got to be quite roughed up inside and I want complete healing from stones and surgery before even THINKING about getting my stent out.
Please advise, thanks.
My husband has solitary kidney and DJ stent is placed 5 time from 2014 to 2018 every time stent is removed his creatinine level rises to dialysis level then doctor place it again we are worried doctors unable to find any obstruction through cystoscopy and urodynamics
Any possible solution?
Join the discussion…
Hello , can you help , I am really nervous and in a lot of pain , I have recently had sepsis after an abcess burst on my kidney, I had stent put into kidney which hasn’t worked and been left in for 8 months, I pass blood every day, only a little and unbearable at times to urinate , I have a urethra stent in me which I have had now for 8 months and supposed to be having another op for laser endopyelotomy to my kidney , should the stent be left that long as I can barely walk and in excruciating pain every day , what do I do if doctors aren’t listening to me?
Hello doctor i have kidney stone and I had operation 23/11/17 they put stent for three months however I would like to remove the stent within one month two weeks is it oky please answer many thanks Ali
Dear sir my bro had a kidney stone .and he done a operation June 26 2017
And the doctor said after 45 days he want to remove the stent but still he didn’t remove.if it create any problem sir
I had a kidney stone size of a quarter had a stent put in on September 12th I had the stone blasted and a stent put in stent came out slightly got very ill with back in had emergency surgery had the stent removed and a stent put back in got very ill because of fever went back in had stent removed and another one put back in doing fine now on October 2nd I will have my stent removed which would be two weeks after it was put in my doctors were fabulous have never had any problems with anything except for having an infection cuz it’s slightly came out but I love my two doctors they did a great job that’s dr. Weedin and Dr Bernard at Kaiser Manteca California thank you you guys you’re fabulous Deborah cuascut
I have had a stent for 3months been urinating blood every since pain unbearable I hate and dred going to pee y we’re people blessed wit stents and stones
I have had a stent in three months urinating blood every since in pain everyday feel like got to go so bad but then only few drops of blood burning and lots of pressure in lower front stomach and lower back so bad y we’re people blessed wit stents and stones
Hello , dr.’s is no care anything , when they put stent , like he did to me , he dont care , how I feel , if I in pain …. ihave stent for about 5 month . After they finely pull out ,I have a pain until now , from 2015 . The stent if sit in body ,very long time , start growing in to body , even its plastic , can you imagine , how its bad for kidney . Dr’s is all fault !!!! if person forget , why DR. no call and remaind to his patient about the pulling the stent ???!!! Its crazy ! Dr’s and farmacys is now world business !! its all ! who care about us. VERY BIG CAREFFUL NOW WHIT DOCTORS !
There is no such thing as the perfect stent. I read a stent should not be left in a patient over 3 to 4 months and could need to be replaced sooner than that.
I am not a doctor & I have a forgotten stent left in my ureter since APRIL 21 2009.
8 years
I do wish you the best on this matter.
You are in my Prayers.
I can’t say my case is negligence, this is crime
How one person like Dr. Can leave sameone a suffering like this 3 years with all this syntoms and pain worrible moments.
All this he have to cover all neglegence he still a give confirmation how as take out my stent,this is bad ,he can imagine my day by day he change my life .
I need help I don’t non how long more I can keep this material in my body,I can dead.
I am 73 years old and in 2001 I was diagnosed with prostate cancer and the radical surgery in October of that year. In January of 2002 scar tissue had developed and I had to have surgery to reopen the urethra. The same occurrence happened again in March of 2016. My doctor at that time recommended me to Dr. Mordkin at Georgetown . We met and he recommended a fairly new procedure which placed a stint inside to keep the passage open. About 3 months later the scar tissue had grown thru the stint and it was recommended that a second stint be inserted. This worked for the most part with the exception that I have had to have two minor surgeries to widen the opening. The problem I have had for the last approximately ten years is the pain from the stints whenever I sit down or have to urinate or have a bowel movement. The pain is sometimes very severe. I have never been told anything about removal .
I recently found a letter stating that my doctor had been trying to reach me so that a stent cold be removed . I believevthatbthis sten was placed in 2002 and I did not see the letter until 2013.
Periodically I get chills , sacral pain , headaches sometimes a fever , lethargy and just feeling ill .
These episodes occur following a UTI and would last intermittently for months or even
Years.
All the specialists I have been to can’t find out what’s wrong . I had a Cystoscopy .Ct scan . I am now wondering if my symptoms could be from an imbedded stent
get all your medical records and that may help you find out
You better do something quick ! My friend just passed away because his stent was left in way too long.He went sepsis overnight.He was only 56 y/o. Don’t wait ! You can’t rely on these doctors .
My mom had a stint put in after gall blade surgery in 2014. She has a recurring uti’s almost every month since. Just two weeks ago she got severely sick and had to be taken to the ER. They sent her home saying she had a uti. A week later I had to the her bacteria to the ER because she couldn’t keep any food down and was severely nasiated. Her doctor told me to take her to a gaterinologist. I did and they drew blood and her lipase levels were 600. They told me to take her to the Er and said her Stent should have been taken out shortly after surgery. Iam so worried about her. They said they will remove the stint tomorrow. Iam so worried will she be alright? What can you do when doctors are so neglegent?
Hi Brenda, my mum is going through a very similar situation, could you please tell me how it went? Was the stent removed without any problems? I am só worries about my mum, please help!
Hi I’m 26 I’M going to have my surgery on Tuesday 17 2015 and I’m really scared because there going take my stent out, they pull me the stent on 2011 so I have more then 3 years with it.. the doctors said that I have a big kidney stone in my bladder and a lot more in my ureter. They did me a CT SCAN but they can see if my stent go stuck . There placing a camera into the bladder (cystoscopy) to directly see and grab the stent with a small grasping device. and brake up of my stones.. I been searching online and I gust I’m the only one that has a stent up to 3years . I’M praying GOD every things comes ok because I have kids.
My name is Yvette Ferrell and ive had a stent in for six years and WHICH is very dangerous and it fell apart in his hands.
I have had a stent 2 years and 4 months and I am scared it’s going to be stuck I have a big kidney stone in each kidney .please help with my questions,email me twyla_lindsey@yahoo.com
Ive had mine for 3 years & just waiting to see the urologist in 2 damn months.
Im kind of scared that its encrusted & attached to my body.
so what happend after surgery? did it come out fine ?
The doctor put me a stent on October 2011 i thought i was going to live with the stent but last year i got alot of pain so i when to the hospital and i explain the doctor i had a stent he ask for how long and i told him and he told me that the stent is only for 3 or 4 months. I didn’t know that . But anyways he referred me to doctor he sends me to Ct scans then i go back to see him and then he makes me another appointment for another. 3 months for another CT scan and i see him again. When i first saw hin i only had one kidney stone now i have more then 8 amd the first one it’sso big now. .. i ddon’t know what to do. .
I got a jj stent how long can I go with it befor I remove it.
don’t have money to do it now
2 to 6 months maximum jj stent life in ureter
my mother now 67 had lithoscopy on 2012 july. after surgery forgot to removed the stent .Now it has been two yrs n again c is facing UTI,PAIN and other problems.went to urologist said stent has fragmented and one end has gone to kidney may nid major surgery . plsss help
bolin
I have had a stent in since october. It was put in because of a 7mm kidney stone. i was told to call back in two weeks to get the stone shattered with the lazer and have the stwnt removed. when i called back i was told we won’t touch you without insurance. is there a different way to go about getting this problem taken care of before it becomes worse. every ins company has a 12 12 rule about pre existing conditions. That means i would have to wait another 12 months before i could be covered.
my dad has had a stent in for over 7 months now he is 81 years old and has constant urine infections since january,and as been in and out of hospital as a result,and as not had his stent changed and as been told he is on a waiting list so this means,the stent will be left in for another 3 months ,could you tell me if this is right.
My husband had a kidney stone, the Dr. did lithotripsy, He also was dignosed as having a small spot of cancer in that kidney June of 2012, He had squemous cell cancer of the lungs June 2008, it has matasized went to his adrenal gland and right kidney. He did 3 months of Chemo, the Dr. says the tumors are smaller now. He also was having problems urinating, Is that bad that the Dr. did the lithotripsy, he also put a stent in his ureter tube going from his kidney to his bladder. He does urinate better now, since he has the stent. The Dr. said He would not remove the stent for 6 months, and then with a replacement. I’m concerned . Could you please advise us as what we should do?
Thank you
Zelma